Identity of mystery pneumonia bug sharpensQuestions raised over readiness for
lethal SARS epidemic.
20
March 2003
HELEN
PEARSON
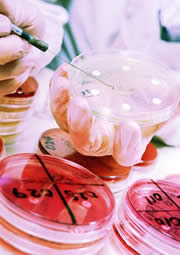 |
| Laboratories have been
comparing the pathogen to known types of
paramyxovirus. |
| ©
Corbis | | |
As laboratories worldwide home in on the virus
responsible for the mysterious global outbreak of
pneumonia, critics say that researchers could have been
better prepared to anticipate the epidemic.
So far, 264 people worldwide are known to have been
infected and 9 have been killed by Severe Acute
Respiratory Syndrome (SARS). This flu-like condition is
characterized by high fever and breathing problems.
Fears began escalating after the World Health
Organization put out an exceptional alert last week.
Laboratories in Hong Kong, Germany and Singapore have
now found signs that the culprit may be a new type of
paramyxovirus - one of a family of viruses that cause
respiratory illnesses, measles and mumps. They examined
the genetic sequence of the virus and looked at its
shape through an electron microscope; both matched those
of known paramyxoviruses.
Immunologists stress that it is too early to conclude
that a paramyxovirus definitely causes the lung illness
- the virus could be a coincidental infection. To be
sure, the collaborating labs must find tell-tale viral
DNA in all patients and show that their blood contains
specific antibodies against the virus.
If the labs' suspicions are correct, there are few
drugs and no vaccine to fight this pathogen, warns
Christopher Broder, who studies paramyxoviruses at the
Uniformed Services University in Bethesda, Maryland. One
drug, ribavirin, could be tried; this is used to treat
the paramyxovirus that causes respiratory syncitial
virus infection in children.
Heads up
New strains of paramyxovirus have killed humans twice
before, after jumping from animals. In 1994, two stable
workers died in Australia having contracted a horse
strain called the Hendra virus. And in 1998, 105
Malaysian pig farmers died from the related Nipah virus.
In both cases, the animals were first infected by fruit
bats.
Events such as these have prompted some experts to
ask why the latest outbreak wasn't better anticipated.
"If we had our act together we could have seen it
coming," says Donald Burke, who studies the spread of
infectious diseases at John's Hopkins University in
Baltimore.
|
If we had our act together we
could have seen it coming |
|
Donald Burke
John's
Hopkins
University
Baltimore | | |
Burke argues that there has been time enough to
develop more rapid diagnostic tests to identify new
strains of paramyxovirus, and to assess potential
strains brewing in animals. "No one is doing anything
approaching a systematic survey of paramyxovirus in
other species," he laments.
These concerns are echoed in a US Institute of
Medicine report co-incidentally issued this week. Its
authors - of whom Burke is one - warn that the world
remains poorly prepared to deal with emerging pathogens.
They call for more investment to boost surveillance and
response to potentially threatening bacteria and
viruses.
Other experts are more sanguine. Infectious-disease
researcher Stephen Morse, of Columbia University in New
York City, reckons that the response to the current
outbreak has been relatively swift and effective. At the
start of the latest epidemic, in February, the Hong Kong
Department of Health traced seven of those initially
infected to the same hotel in Kowloon.
And the spread of the disease seems to have been
partly stemmed by keeping suspected patients in
isolation. So far it is mainly close family members and
hospital workers who have been infected. Even so, the
situation is "damned scary", concedes influenza
researcher Robert Webster of St Jude's Children's
Research Hospital in Memphis, Tennessee. | 

